| Patriot Outreach Supporting all Military Service Men, Women, Retirees, Veterans, Government Civilians, Battlefield Contractors and their Families. |
| Home | My Story | Get Help | What's Happening | About Stress & PTSD | News & Reports | Donate | Mission | Contact |
FM 22-51
LEADERS' MANUAL FOR COMBAT STRESS CONTROL
CHAPTER 5
BATTLE FATIGUE
5-1. Introduction
Battle fatigue is the approved US Army term (AR 40-216) for combat stress symptoms and
reactions which --
- Feel unpleasant.
- Interfere with mission performance.
- Are best treated with reassurance, rest, replenishment of physical needs, and activities
which restore confidence.
a. Battle fatigue can also be present in soldiers who have been physically wounded or
who have nonbattle injuries or diseases caused by stressors in the combat area. It may be
necessary to treat both the battle fatigue and the other problems.
b. Battle fatigue may coexist with misconduct stress behaviors. However, battle fatigue
itself, by definition, does not warrant legal or disciplinary action.
c. Several of our allies use other terms for battle fatigue such as combat reaction, combat
stress reaction, or battle shock.
5-2. Contributing Factors Which Cause Battle Fatigue
There are four major contributing factors which cause battle fatigue. They are --
- Sudden exposure.
- Cumulative exposure.
- Physical stressors and stress symptoms.
- Home front and other existing problems.
Any one factor may suffice if intense enough. Usually two, three, or all four factors can
collectively produce battle fatigue.
5-3. Signs/Symptoms of Battle Fatiguea. The first factor is the sudden exposure or transition to the intense fear, shocking
stimuli, and life-and-death consequences of battle. This occurs most commonly when
soldiers are committed to battle the first time but can happen even to veteran soldiers
when they come under sudden, intense attack. Soldiers in "safe" rear areas may be
overwhelmed by the horrible stimuli and consequences of war without themselves being
under fire. This is an occupational hazard for rearward command and support personnel,
including medical.b. The second factor is the cumulative exposure to dangers, responsibilities, and horrible
consequences. Exposure can cause repeated grief and guilt over loss of fellow soldiers. It
can also give the sense that one's own luck, skill, and courage have been used up. The
rate of accumulation depends on the rate of losses (KIA, WIA, died of wounds [DOW],
and other causes) and of "close calls" with disaster and death (including being wounded
oneself). Periods of rest, recreation, and retraining in which new supportive, cohesive
bonds are formed may temporarily reverse the accumulation but not stop it completely.
c. The third factor is the physical stressors and stress symptoms which reduce coping
ability. Sleep loss and dehydration are especially strong contributors. Also important are
physical overwork, cold, heat, wetness, noise, vibration, blast, fumes, lack of oxygen,
chronic discomfort, poor hygiene, disrupted nutrition, low-grade fevers, infections, and
other environmental illnesses. These stressors are also in the area of responsibility of
preventive medicine. In moderate amounts, such physical stressors contribute to battle
fatigue but are reversed by rest and time for restoration. In higher doses, they cause
serious illness or injury requiring specific medical or surgical treatment. When the major
contributing factors to battle fatigue are physical stresses that can be reversed, treatment
is usually simple and recovery is rapid. However, physical factors are not necessarily the
cause of battle fatigue. When the soldier is diagnosed, the absence of obvious physical
stressors should not detract from the positive expectation of rapid and full recovery.
d. The fourth factor is the home front and preexisting problems.(1) Israeli studies found that the strongest factor which distinguished between
soldiers who were decorated for heroic acts and those who became battle shock
casualties was having had many recent changes on the home front. The negative
home front problem may be a "Dear John" letter, a sick parent or child, or bad
debts. Or it may be something positive -- being recently married or becoming a
parent. Worrying about what is happening back home distracts soldiers from
focusing their psychological defenses on the combat stressors. It creates internal
conflict between performing their combat duty and perhaps resolving the home
front problems or concerns.
(2) The second strongest factor found in the Israeli studies was unit cohesion: the
soldiers who became stress casualties were often committed to battle alongside
strangers, while those who became heroes were alongside unit members they
knew well, trusted, and depended on. These findings confirm observations from
previous wars. Other baseline stressors which are often cited include lack of
information; lack of confidence in leaders, supporting units, or equipment in
comparison with the enemy's; and lack of belief in the justness of the war (which
may reflect lack of support for the effort in the US).
(3) It is worth noting that individual personality makeup does not predict
susceptibility to battle fatigue. Careful studies by the US Army after WWII and
by the Israelis since the Yom Kippur War all show that there is no clear
relationship between neurotic traits or personality disorders and battle fatigue.
People with these traits were no more likely to become battle fatigue casualties
and no less likely to be decorated for valor than were those soldiers who tested as
normal.
(4) There are personality factors which may predict who will be poor soldiers (or
who may be prone to commit acts of misconduct if given opportunities or excuses
to) but not who will get battle fatigue. There are good predictors of battle fatigue
but individual personality type is not one of them. Anyone may become a battle
fatigue casualty if too many high-risk factors occur. However, personality factors
may help predict who is less likely to recover quickly after being disabled by
battle fatigue.e. There are two common themes which interact in varying combinations in most battle
fatigue casualties -- loss of confidence and internal conflict of motives.(1) Battle-fatigued soldiers have often lost confidence in --
- Themselves -- their own strength, alertness, and abilities, or the adequacy
of their training.- Equipment -- their weapons and the supporting arms.
- Buddies -- other members of the small unit, or in the reliability of
supporting units.- Leaders, to include --
- The skill and competence of the small unit leader or the senior
leadership.- Whether the leaders care about the soldiers' well-being and
survival.- The leader's candor (honesty) or courage.
These doubts, plus the soldiers' estimate of the threat situation, raise questions
about their chances of surviving and/or of succeeding with the mission. Loss of
faith in whether the "cause" is worth suffering and dying for also plays a role. It
has been said that soldiers join the military services for patriotism, but they fight
and die for their buddies and trusted leaders. Soldiers do not want their comrades
or themselves to die for an unjust cause or for other's mistakes. Loss of faith may
even spread to a painful loss of belief in the goodness of life and other spiritual
and religious values.
(2) Combat, by its nature, creates conflicts between motives within an individual.
The desire for survival and comfort is in conflict with the fears of failure or
disgrace and the soldier's loyalty to buddies. Leaders' actions must --
- Raise the soldiers' confidence.
- Help resolve the soldiers' internal conflict in favor of his sense of duty
a. Simple Fatigue. The simple fatigue or exhaustion form of battle fatigue is normally the
most common. It involves tiredness, loss of initiative, indecisiveness, inattention, and,
when extreme, general apathy. These cases may show some features of the other forms,
especially anxiety and pessimism, but not to the degree that they cannot rest and recover
in their own unit (duty) or in a nonmedical support unit (rest). However, the tactical
situation may call for them to rest in medical cots if no other suitable place is practical.
b. Anxious. The anxious form is naturally one of the most common, given the danger of
combat. Symptoms include verbal expressions of fear; marked startle responses which
cease to be specific to true threat stimuli and become generalized; tremor; sweating; rapid
heartbeat; insomnia with terror dreams, and other symptoms of hyperarousal. This form is
often seen while the soldier is close to the danger and shifts to the exhausted or depressed
forms as he is evacuated towards the rear.
c. Depressed. The depressed form is also common. It may have the slowed speech and
movement of the simple fatigue form or the restlessness and startle responses of the
anxious form. The depressed form also has significant elements of self-doubt, self-blame,
hopelessness, and may include grief and bereavement. The soldier may be pessimistic
about the chance for victory or survival. The self-blame and guilt may be about perceived
or actual failures in the combat role or mistakes made. It may be related to home front
issues. Or it may be relatively pure survivor guilt -- the irrational feeling of a survivor
that he should have died with members of his unit or in place of a buddy.
d. Memory Loss. The memory loss form is usually less common, especially in its extreme
versions. Mild forms include inability to remember recent orders and instructions. More
serious examples are loss of memory for well-learned skills or discrete loss of memory
for an especially traumatic event or period of time. Extreme forms include disorientation
and regression to a precombat (for example, childhood) state. Total amnesia, or a fugue
state in which the soldier leaves the threatening situation altogether, forgets his own past,
and is found wandering somewhere else (having taken on another superficial identity),
can also occur. Physical causes of amnesia such as concussion or substance misuse (for
example, alcohol) must be ruled out in such cases.
e. Physical Function Disturbance. Disturbance of physical function includes disruptions
of motor, sensory, and speech functions. Physical injuries or causes are absent or
insufficient to explain the symptoms.
- Motor disturbance includes --
- Weakness or paralysis of hands, limbs or body.
- Sustained contractions of muscles (for example, being unable to straighten
up or to straighten out the elbow).- Gross tremors; pseudoconvulsive seizures (sometimes with loss of
consciousness).- Visual symptoms may include --
- Blurred or double vision.
- Tunnel vision.
- Total blindness.
- Auditory symptoms may involve --
- Ringing (or other noises) in the ears.
- Deafness.
- Dizziness.
- Tactile (skin) sensory changes include --
- Loss of sensations (anesthesia).
- Abnormal sensations, such as "pins and needles" (paresthesia).
- Speech disturbance may involve --
- Stuttering.
- Hoarseness.
- Muteness.
(1) The physical symptoms often begin as normal but transitory incoordination,
speech difficulties, or sensory disruption. These symptoms are triggered by
physical events, such as explosions, mild concussion, or simple fatigue. They are
magnified when emotions cannot be expressed because of social pressure or
heroic self-image. They are, therefore, most often seen in the "elite" units or
groups who show few other cases of battle fatigue, such as officers or the airborne
and rangers in WWII. They are also more common in individuals from social
classes and cultures that receive less education and/or do not learn how to express
feelings in words.
(2) In some cases, the physical "disability" may have a clear symbolic relationship
to the specific emotional trauma or conflict of motivation which the soldier has
experienced. The disability may make the soldier unable to do his job and so
relieve him from danger, such as classic "trigger-finger palsy." The symptoms
may be reinforced by reducing his anxiety and eliminating internal conflict of
combat duties. Symptoms also may be reinforced by receiving the relative luxury
of rear area food, hygiene, and sleep. However, not all cases fit that pattern. Some
soldiers with significant loss of function from battle fatigue have continued to
perform their missions under great danger. Medical personnel must be alert to
new physical forms of battle fatigue which mimic physical injury, such as might
be attributed to lasers, radiation, or chemical agents.f. Psychosomatic Forms. These psychosomatic forms of battle fatigue commonly present
with physical (rather than emotional) symptoms due to stress. These include --
- Cardiorespiratory --
- Rapid or irregular heartbeat.
- Shortness of breath.
- Light-headed.
- Tingling and cramping of toes, fingers, and lips.
- Gastrointestinal
- Stomach pain.
- Indigestion.
- Nausea/vomiting.
- Diarrhea.
- Musculoskeletal --
- Back or joint pain.
- Excessive pain and disability from minor or healed wounds.
- Headache.
According to some WWII battalion surgeons, the psychosomatic form of battle fatigue
was the most common form seen at battalion level. This type of case may have accounted
for a large percentage of all patients seen at battalion aid stations (BASs) during times of
heavy fighting.
g. Disruptive Forms. Disruptive forms of battle fatigue include disorganized, bizarre,
impulsive or violent behavior, total withdrawal, or persistent hallucinations. These are
uncommon forms of battle fatigue, but they do occur. Battle fatigue symptoms are a
nonverbal way for soldiers to communicate to comrades and leaders that they have had
all they can stand at the moment. Battle fatigue takes on whatever form the soldiers
expect. It is important, therefore, to create positive expectancies and to eliminate the
belief that battle fatigue soldiers usually do crazy, senseless, or violent things. Leaders,
medics, and combat stress control personnel must ensure that battle fatigue casualties are
never referred to as psychiatric casualties.
5-4. Labeling of Battle Fatigue Cases
a. As stated earlier, battle fatigue is the US Army approved label for this condition.
Fatigue implies that it is a normal condition which can occur in anyone who is subjected
to the extreme mental and emotional work of combat missions. Fatigue also implies that
it gets better quickly with rest. The term should be applied to the normal but
uncomfortable reactions to combat stress. It should also be used with the more seriously
impairing responses in order that it not take on the connotations of breakdown or a
release from duty. However, some cases do require treatment in medical facilities, skilled
counseling, and even brief tranquilizing or sedative medication.
b. Historical experience proves that it is important not to try to make early distinctions
among battle fatigue cases based on presumed causes and likely response to treatment.
Cases due to acute emotional stress versus subacute physical stress versus chronic
cumulative stress may need somewhat different treatment. These cases have, on the
average, different likelihood for successful return to duty. However, these battle fatigue
cases may be quite impossible to distinguish at first by their appearance and symptoms.
Accurate individual history may be unattainable during battle and especially during the
first interviews. All cases should, therefore, be called battle fatigue and be treated
immediately with positive expectation of rapid, full recovery, as close to their units as the
tactical situation permits. It is essential to avoid dramatic or medical/psychiatric labels for
this condition.
CAUTION
Do not prejudge whether a battle fatigue soldier will recover quickly or slowly based
on initial appearance. The symptoms are very changeable. Do not rely on initial
information about the relative contributions of acute emotional stress, physical
fatigue, chronic exposure, or baseline factors. The incomplete history may be
misleading.
(1) Consider each contributing factor in designing treatment.
(a) How to reassure.
(b) How much rest.
(c) What to replenish first and most.
(d) What activities to assign to restore confidence.
(2) Keep positive expectation for recovery.
(3) Get more validated information from the rested soldier and the unit.
(4) Revise the plan based on response to treatment.
c. Battle fatigue may occur in anticipation of the action, during the action, or after the
action (during lulls when sick call is again possible or when the unit returns to a safe rear
area). Usually, the rise in battle fatigue casualties is preceded by 1 to 3 days of increases
in the number of soldiers wounded and killed. All of these cases are still called "battle
fatigue" as long as the soldiers are in the theater of operations and are expected to recover
and return to duty. The terms conflict fatigue, crisis fatigue, stress fatigue, or field fatigue
may be used for peacetime cases which are reactions to intense mission stressors but do
not involve actual battle or life-and-death consequences. These cases should be treated
the same way as battle fatigue with no negative connotations.
d. Sublabeling of battle fatigue cases is based solely on where they can be treated. Hence,
sublabels depend as much on the situation of the unit as on the symptoms shown by the
soldier. The labels light and heavy, duty and rest, hold and refer, when added to the label
battle fatigue, are nothing more than a short-hand or brevity code for saying where the
soldier is being treated or sent. They have no other meaning and only transient
significance. The sublabel should be updated as the soldier improves or arrives at a new
echelon of care.
e. Figure 5-1 diagrams the choices that lead to the several sublabels for battle fatigue
cases
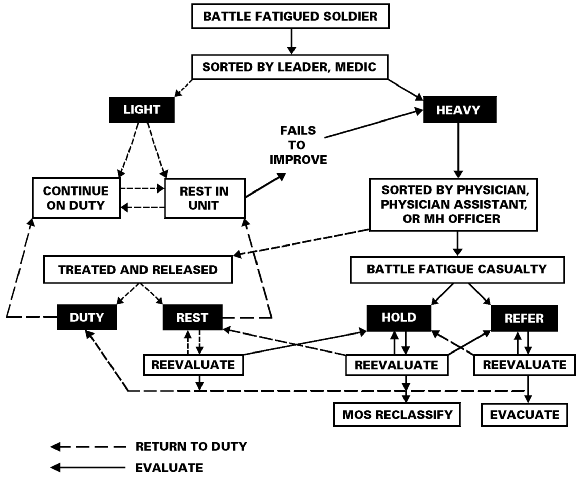
Figure 5-1. Diagram of sorting choices and labels for battle fatigue cases.
(1) Light battle fatigue can be managed by self and buddy aid, unit medics, and
leader actions. Most soldiers in combat will have light battle fatigue at some time.
This includes the normal/common signs of battle fatigue listed in the Graphic
Training Aid (GTA) 21-3-4 (available from US Army Training Audiovisual
Support Centers). Light battle fatigue also includes the warning (or more serious)
signs listed in GTA 21-3-5, provided the signs respond quickly to helping actions.
Soldiers with these symptoms do not need to be sent immediately for medical
evaluation and can continue on duty. If the symptoms persist after rest, they
should be sent to their unit surgeon or physician assistant at routine sick call as
heavy.
(2) Heavy battle fatigue (previously called severe) deserves immediate medical
evaluation at a medical treatment facility. The symptoms may be --
- Temporarily too disruptive to the unit's missions.
- A medical/surgical condition which requires observation and diagnosis to
rule out the necessity for emergency treatment. The medical triager sorts
the heavy battle fatigue soldiers based on where they can be treated.(3) Duty cases (previously called mild) are those who are seen by a physician or
physician assistant but who can be treated immediately and returned to duty in
their small unit.
(4) Rest cases (previously called moderate) must be sent to their unit's nonmedical
CSS elements for brief rest and light duties; rest cases do not require continual
medical observation.NOTE
Duty and rest cases are not medical casualties because they are still available for
some duty in their units. However, those heavy cases who cannot return to duty or
rest in their unit the same day are battle fatigue casualties.
(5) Hold cases are those who can be held for treatment at the triager's own
medical treatment facility because both the tactical situation and the battle fatigue
casualties' symptoms permit. This should be done whenever feasible.
(6) Refer cases are those who must be referred (and transported) to a more secure
or better-equipped medical treatment facility, either because of the tactical
situation or the battle fatigue casualties' symptoms. Refer becomes hold when the
soldiers reach a medical treatment facility where they can be held and treated.
NOTE
The hold and refer sublabels of heavy battle fatigue do not necessarily mean that a
soldier is less likely to recover or will take longer to recover than cases treated as
rest. However, the simple fact of holding or evacuation itself often prolongs the
treatment and decreases likelihood of full recovery and return to duty.f. There is no easy rule for deciding whether any specific symptom of battle fatigue
makes the soldier a case of duty, rest, hold, or refer battle fatigue. That will require
judgment based on --
- What is known about the individual soldier.
- The stressors involved.
- How the soldier responds to helping actions.
- What is likely to happen to the unit next.
- What resources are available.
Battle fatigue symptoms can change rapidly based on a soldier's expectations. A
successful combat stress control program prevents unnecessary evacuation and shifts
battle fatigue cases from refer to the hold combat neuropsychiatric triage category. More
importantly, it shifts many soldiers from hold category to rest and duty category. This
allows them to recover in their units and keeps them from overloading the health service
support system.
5-5. Severity of Symptoms and Response to Treatment
a. The severity of symptoms and the speed and extent to which they respond to treatment
are directly related to the intensity, lethality, and duration of the battle incidents which
caused them. The following are general planning estimates which may be modified
greatly by specific factors, such as unit cohesion, training, and leadership.
b. Leader and medical personnel in forward areas should expect as many or more soldiers
to present with duty or rest battle fatigue as there will be hold and refer cases. It is
essential that the former not become casualties by unnecessarily evacuating or holding
them for treatment.
c. In general, the more intense the combat, especially with indirect fire and mass
destruction, the more cases become heavy and need holding or referral, and the harder it
is for them to recover quickly and return to duty.
d. Fifty to eighty-five percent of battle fatigue casualties (hold and refer) returned to duty
following 1 to 3 days of restoration treatment, provided they are kept in the vicinity of
their units (for example, within the division).NOTE
When returned to their original units after successful treatment for battle fatigue, soldiers
have no increased risk of relapse compared to their buddies who have not yet had battle
fatigue. New soldiers who suffer battle fatigue during their first combat exposure deserve
a second chance under supportive circumstances. They are no more likely to breakdown
again than is another new replacement. However, it must be noted that treatment for
battle fatigue will not turn a previously poor soldier into a good soldier. Soldiers who
have accumulated too many terrible experiences may also reach a stage where
reassignment to less dangerous duties is advised.
The variation of success rates between 50 and 85 percent can be due to several factors
besides the intensity of the combat. Combat stress control planners must evaluate them
critically. An 85 percent restoration rate could be the result of effective far forward
treatment of true hold cases. Alternatively, it could occur because many easily treated
cases are being held and rested in medical cots (and classified as hold) instead of being
released to their units as duty or rest battle fatigue. That situation, in turn, could be due
either to inadequate training and consultation to forward units or to a tactical situation
which prevents maneuver units from resting any marginally effective soldiers.
e. Fifteen to fifty percent of battle fatigue casualties do not recover within 72 hours. The
wide variation is due both to the intensity and nature of the battle and to the availability
of far forward treatment. A large number of these battle fatigue casualties (10 to 40
percent of the original total) do return to some duty within 1 to 2 weeks. This is
accomplished only if they continue structured, equally positive treatment. This treatment
may be provided in a non-hospital like atmosphere of a medical treatment (tactical)
facility in the combat zone. Premature evacuation of battle fatigue soldiers out of the
combat zone must be prevented as it often results in permanent psychiatric disability. If
the tactical situation permits, the evacuation policy in the corps should be extended from
7 to 14 days for the reconditioning program, as this will substantially improve the
returned to duty rate and decrease subsequent chronic disability.
f. Five to fifteen percent of battle fatigue casualties fail to improve sufficiently to return
to duty in the combat zone. Further reconditioning treatment can return many of these to
useful duty in the COMMZ. Final evacuation to CONUS should not exceed 5 percent of
total battle fatigue casualties. In retrospect, many of these soldiers have preexisting
personality types or other neuropsychiatric conditions which did not make them become
battle fatigue casualties in the first place but did interfere with full recovery. A lesson
plan on how to identify, treat, and prevent battle fatigue is provided in Appendix E.
Go to Chapter 6 - Post-Traumatic Stress Disorder
FM 22-51
LEADERS' MANUAL FOR COMBAT STRESS CONTROL
Table of Contents
Preface
Chapter 1 - Overview of Combat Stress Control
Chapter 2 - Stress and Combat Performance
Chapter 3 - Postive Combat Stress Behaviors
Chapter 4 - Combat Misconduct Stress Behaviors
Chapter 5 - Battle Fatigue
Chapter 6 - Post-Traumatic Stress Disorder
Chapter 7 - Stress Issues in Army Operations
Chapter 8 - Stress and Stressors Associated with Offensive/Defensive Operations
Chapter 9 - Combat Stress Control in Operations other than War
Chapter 10 - War and the Integrated (Nuclear, Biological and Chemical) Battlefield
Chapter 11 - Prevention of Battle Fatigue Casualties and Misconduct Stress Behaviors
Appendices
Appendix A - Leader Actions to Offset Battle Fatigue Risk Factors
Appendix B - Organization and Functions of Army Medical Department Combat Stress Control Units
Appendix C - United States Army Bands
Appendix D -The Unit Ministry Team's Role in Combat Stress Control and Battle Fatigue Ministry
Appendix E - Example Lesson Plan
Glossary - Abreviations and Acronyms
References - Sources Used
Write to us at Patriot Outreach, PO Box 601, Selma, OR 97538
or
Call Toll Free: 1-866-96-STRONG (866-967-8766) (8am to 4pm Pacific Time) Email: info@PatriotOutreach.org
Copyright 2006-2011 Patriot Outreach